The Post Thrombotic Syndrome is something that can occur after one has experienced a DVT. The acute threat of a thrombosis is a clot going to the lung and heart and subsequent death. However, 95%-97% of people survive a DVT, but often the long term sequelae are not prevented nor adequately treated.
When one has thrombus (clot) in the vein the reason for giving a blood thinner is to prevent the thrombus from breaking off and going to the heart or the lung – it does not necessarily dissolve the clot. As time passes a thrombus becomes matured and forms a type of scar tissue in the vein. This type of blockage is very different from blockages in the arteries.
A thrombus may completely, dissolve, may only partially dissolve causing narrowing of the veins and poor flow or it may damage valves in veins causing ‘backflow’ of blood in the wrong direction. In some people it causes a combination. These changes usually occur from 6 months to 2 years after having a deep vein thrombosis. They can significantly affect quality of life.
These changes may result in the following changes in the legs:
- Swelling
- Varicose veins
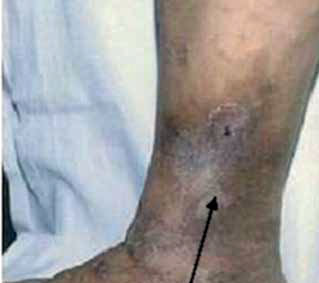
- Hyperpigmentation
- Hardened (sclerotic) skin
- Wound formation
This is from high venous pressure, lack of oxygen and inflammation. It may cause chronic pain, heaviness and throbbing and in extreme cases venous claudication (pain when walking or exercising as though the leg wants to burst as it cannot drain enough blood. This chronic discomfort has been shown to negatively affect quality of life.
Types of PTS
- Leg swelling
- Venous ecstasia
- Hyperpigmentation
- Skin damage and wound formation.
Treatment
The best treatment is prevention! Once one has been diagnosed with a DVT, graduated class 2 or even 3 compression stockings should be worn. Patients should be measured for these and taught how to apply them properly. Should there be a lot of swelling they should be worn daily (while applying gravity to the limbs…so whenever one is upright) and they should be changed every six months as stockings lose their elasticity.
Sometimes surgical procedures can be done to improve flow. These usually entail Vein Stenting.